This case scares me. Truly. We have all had patients with this chief complaint, maybe on a weekly, if not daily, basis. You know the one – guy comes in, says he has been diagnosed with …. lets see, its usually “herniated disk”, “muscle strain”, “sciatica”, or he may throw out a term that gets more of your attention like “stenosis”, but usually it’s just “I have a bad back” and now on narcotics (because there’s just no other way – ugh!) and just needs a refill. He may even have an empty bottle in hand. He just might ask for the medicine by name : “Norco 10s work really well, but my doctor put me on Oxycontin now. Can you give me enough for a month?” Response: “uh… No.” But I digress…..lets go to our crazy-scary case…
Category Archives: SonoCases
SonoCase: 72 yr old, woke up with “funny” vision… What’s up with that eye?!
One of my good friends and colleagues, Dr. Graham Walker, emailed me the other day with a “booya, check it out”-type of email that he knows I love and cherish. He made the diagnosis quickly with the help of his bedside US study.
72 year old male with a history of hypertension, high cholesterol and on antibiotics for a foot infection – – stating he woke up and his vision was “funny” – Continue reading
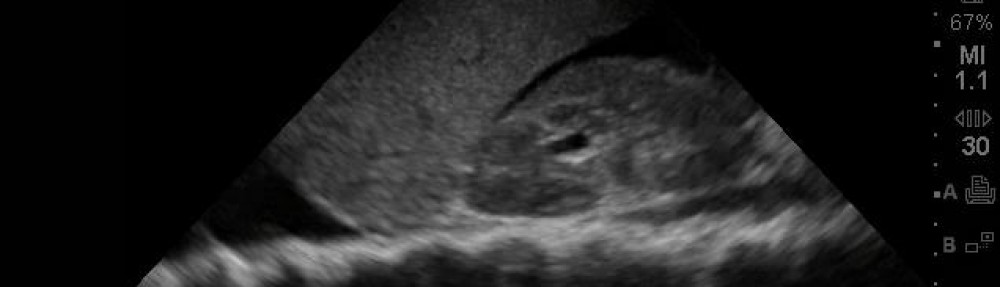
SonoCase: 2 yr old walking into things, now cups his eye to focus…. What’s up with that eye?!
Very cool pick-up we had recently, the early diagnosis allowed better outcome, and I’ve only seen this twice before by bedside US in the ED. It was an unusually calm Monday in the pediatric ER, lots of coughs and colds, and more hand-foot-mouth disease than ever recorded in history, Im sure. Then we saw this very cute 2 year old boy walk into the ER wearing a “Poop happens” T-shirt, with his hand covering his left eye while walking to the room, then hopping on the gurney and immediately taken by the iPAD we have for kids to play games on…. Continue reading
SonoCase: 45 yr old female acute respiratory distress…. RUSH, part deux
Here’s another crazy case I had in the middle of the night in the ED, a night that was particularly… let’s say… challenging. Lots of patients (about 43 actually) and 2 thankfully great residents, and one other ED attending. We were busy supervising a chest tube placement, while overseeing the trauma next door and finishing our charts on other patients so they can be dispo’d (yup, multi-tasking at its best – [or worst, ya never know]) and we get a ring down of a 45 year old in acute respiratory distress placed on non-rebreather with subsequent vitals: HR 130s BP 80s/50 RR 38 90%O2 sat. Continue reading
SonoCase: 78 yr old, hypotensive, altered…Welcome to “RUSH” week!
Yup, that’s right, we are going to go through the RUSH exam this week. Its “RUSH” WEEK!!!! To all those in SonoSororities and SonoFraternities out there, this week is going to be dedicated to “rush”ing to evaluate the patients in shock, and trying to figure out the cause of it by your handy-dandy bedside US machine – especially when the case is not obvious, but you know you need to “rush” to their bedside….ok, Ill stop “rush”ing 🙂
RUSH stands for Rapid US in SHock and written by great friends of mine, namely Phil Perera, Tom Mailhot, D Riley, and Diku Mandavia who coined the terms Pump-Tank-Pipies – with inspiration from an original RUSH protocol by another great friend of mine, Scott Weingart (aka emcrit) who coined the acronym HIMAP (heart, IVC, Morison’s (and other FAST views), Aorta, Pneumothroax (see a great podcast by him here). Both start with the heart, and for good reason – you may find the cause immediately, and you’ll be able to identify if the patient can tolerate fluids. Both also arose from varying research studies by Rose et al. (the UHP protocol) and by Bahner et al (Trinity protocol) and Lichtenstein’s FALLS protocol (see thebluntdiessection’s article). Here, we will discuss the 3 sections to evaluate:
SonoStudy (and Case): 53% of septic patients’ treatment plans changed after seeing the IVC and cardiac contractility
The study coming out in Annals of Emergency Medicine in June done by Haydar et al “found point-of-care ultrasonographic data about cardiac contractility, inferior vena cava diameter, and inferior vena cava collapsibility to be clinically useful in treating adult patients with sepsis” – for those of us who use US regularly to evaluate patients in shock, whether it’s by using the RUSH protocol or evaluating the initial and post-fluid volume status for those we are trying to resuscitate when septic, it’s no big surprise. What is the surprising aspect of this is that 53% of septic patients’ treatment plans had changed due to the findings by ultrasound of cardiac contractility and IVC appearance. Continue reading
SonoCase: 25 yr old positional, pleuritic, chest pain. “It’s just pericarditis” Really?
Had a great case the other week of a patient who was previously healthy (“great” because of what it reminds us all to do with this diagnosis) , and other than a girlfriend who he fought with too frequently causing him to go into panic attacks and hyperventilate, he doesn’t have any other stressors in his life – psychologic or drug-induced (yes, I mean cocaine). He came to the ED c/o positional chest pain, worse when lying flat and breathing in, has been persistent for over a week with a recent viral syndrome but no current fever, cough or respiratory distress. He looked well, but felt tired, had no energy to walk a few blocks and that has been worsening over the week, which is when he got into another fight with his girlfriend about coming into the ED for evaluation. Thankfully, he lost and came in. Continue reading
SonoCase (and studies): Renal colic, do we really need to get another CT?
38 year old male with a history of kidney stones c/o severe right flank pain, radiating to the groin, “feels just like my kidney stones” with small amount of blood in his urine, begging for pain meds. Ok, I know this is not the most mysterious case, but when I looked over his chart he has a radiology list of 8 CT scans over the last 5 years to evaluate for kidney stones! Why? Do we really work in an era where we MUST know the diagnosis instead of just being able to screen for the emergent conditions, and treat by using our clinical judgement… and bedside ultrasound? I sure hope not, because that’s not how I practice. This is not the first-time flank pain patient, although some would argue that you dont need to get a CT for that either if labs and ultrasound are clear/negative. This is also not the elderly patient that could have belly-badness that will die soon – but not from CT scan-radiation-induced cancer, that’s for sure. Continue reading
SonoCase: Motorcycle victim: needs OR! But wait…
So, this case that I just had the other day is an example of an “oldy but goody” reason why bedside ultrasound rocks, especially in the blunt trauma victim with multiple injuries. 40 year-old motorcycle helmeted driver going moderate speed was T-boned by a car and fell onto his left side. He c/o severe left leg pain and mild left lower back pain, with STABLE (and yes, I mean, stable/normal/not worrisome vitals – HR 72, RR 16, BP 148/90, O2 sat 97%RA) with a clear primary trauma survey, and a secondary that revealed a small abrasion on his cheek, no left sided chest wall tenderness, nontender abdomen, no pelvis instability, an obvious deformed open fracture of his left tibia/fibula, and left lower posterior rib cage tenderness without crepitance or bruising. An E-FAST was done… Continue reading
SonoCase: Pediatric lower abdominal bulge? What the…?
You know, working in the pediatric ER is always a joy since most children are going to do well (and most parents are worry warts – but who am I kidding, I would be too!). But sometimes I get a case that surprises me – and this is one of them. Of course, in hindsight, it makes sense, but still interesting given the way the kid presented: 4 year old boy, with a history of “retractable bulges a few years ago” comes to the ER after his mom noticed that he woke up that morning (4 hours prior to arrival) walking funny. She took down his very cute Star Wars pajama pants and saw this: