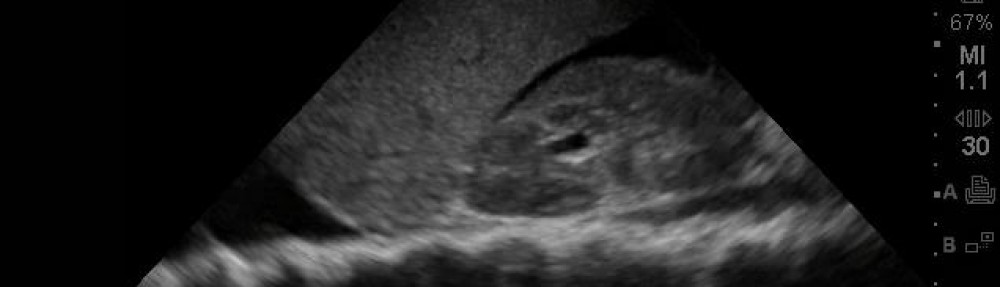
Whenever you are performing an E-FAST exam on your trauma patient or a thoracic US in those with unexplained shock or shortness of breath, your sphincter tightens when you see fluid in the belly or when there is no lung sliding. Ever placed your probe on the left anterior chest wall and have been surprised after noticing there is no lung sliding? Or, that you see this weird movement of “the lung” on the left side, which surely isn’t normal and definitely deeper than the pleural line and you think, “There’s a left pneumothorax!” Well, guess what guys and gals, it just could be the heart. Continue reading
Category Archives: SonoExtras
SonoFiler: Profiling Dr. Vicki Noble
The next edition of the Sonofiler – profiling a leader in bedside US – is going to be about a person who I admire immensely, has truly changed the way others perceive bedside US, and who was a great president of the ACEP US section: Dr. Vicki Noble – or as we call her “Queen Vicki” – because she keeps a straight face when she needs to and perfectly describes the best utility for bedside US (especially in response to the haters out there… and we all have heard and read what they say). Her response to any and all criticism is always honest and clear – she is my hero. I sent VIcki a few questions, and the answers are so honest, humble, and selfless (and not surprisingly spunky too). They are a true testament as to why she is one of the leaders in bedside US. So let’s talk about how I know that… Continue reading
SonoNews: ASA Guidelines for central venous access now includes ULTRASOUND!
Now I know that many of you may already be using ultrasound to help guide your needle when obtaining central venous access, but when a governing body announces its importance, it’s a big deal! If any of you are like me, you learned how to place all central lines using the “blind” technique – despite your eyes being wide open – but now that the ultrasound machine is your eyes beneath the skin, there is no longer a reason to be so blind about it! Isn’t it nice to know where “big red” is? Here, I’ll answer for you – Heck YEAH! So why am I excited? Well… Continue reading
SonoCase (and studies): Renal colic, do we really need to get another CT?
38 year old male with a history of kidney stones c/o severe right flank pain, radiating to the groin, “feels just like my kidney stones” with small amount of blood in his urine, begging for pain meds. Ok, I know this is not the most mysterious case, but when I looked over his chart he has a radiology list of 8 CT scans over the last 5 years to evaluate for kidney stones! Why? Do we really work in an era where we MUST know the diagnosis instead of just being able to screen for the emergent conditions, and treat by using our clinical judgement… and bedside ultrasound? I sure hope not, because that’s not how I practice. This is not the first-time flank pain patient, although some would argue that you dont need to get a CT for that either if labs and ultrasound are clear/negative. This is also not the elderly patient that could have belly-badness that will die soon – but not from CT scan-radiation-induced cancer, that’s for sure. Continue reading
SonoStudy: US-Guided Nerve Blocks – in disasters, your ED, and your hearts
Given this memorial day weekend, and the sacrifice of our troops, lets discuss something that the military has used for years – and for good reason. US-guided nerve blocks are becoming more and more utilized in our EDs. Especially when we have the elderly patient who is in severe pain from a humeral fracture or a femoral neck fracture, and you’d rather not have to watch (and chase) their blood pressure after giving systemic opiates. It is also a great resource in resource-poor areas, like the aftermath of the disaster of the Haiti earthquake. This is all clearly discussed in the article in Annals of Emergency Medicine this month by Drs. Suzanne Lippert, Arun Nagdev, Mike Stone, Andrew Herring, and Robert Norris. Continue reading
SonoTip&Trick: “I can never get a nice subxiphoid view!” Really? Well try this…
You get a patient who has gradual onset of shortness of breath with a history of cancer, a patient with sudden severe exertional chest pressure and new orthopnea, a patient with known pericarditis with worse pain or breathing difficulty, or a trauma patient with a penetrating stab wound to the chest and you want to evaluate whether they have a pericardial effusion, signs of tamponade, or poor contractility through a bedside echo, but you just can’t seem to obtain a great subxiphoid (SX) view. The SX view of the heart seems like it would be easy to obtain. I mean, it is right there! – right by the probe, and the patient is alive so you know he has a heart! Well, sometimes it’s not so easy. There are several reasons for this: your probe positioning, not seeing the liver, and the patient’s thoracic cage.
SonoNews: EM Milestones from the ACGME report are in!: Go Ultrasound!!
EM Milestones came out and just heard from SAEM that ULTRASOUND is one of them!!! Nicely done everyone! Scroll down to P12 to read through the bedside goal-directed ultrasound section. http://www.saem.org/sites/default/files/EM_Milestones_ABEM_Final.pdf
SonoLinks: The websites, smartphone apps you need to know for Bedside US
A list of awesome sites and apps for bedside US: whether that be for viewing lectures, US videos/images of normal/abnormal pathology, learning the technique for each application, or to get all that you need to know on your smartphone – you’ll love these! This is not a complete list, but ones that I have found to be great! If you know of any others, feel free to list in the comments.
ACEP US Section – for all the needs of emergency physicians who perform US, credential others, direct US programs and much more!
SAEM US Academy – is a community within the Society of Academic Emergency Medicine. AEUS provides an international forum bringing together bedside clinician sonologists with the common goal of advancing patient care
Bedside US and the Stanford 25 – The Stanford 25 is a list of 25 dependent physical diagnosis maneuvers to help with the physical exam and medical education, one of which is bedside US
Society of US in Medical Education – this link takes you to the learning modules, but if you press “Home” you will see how amazing this society is for enhancing US education.
Emergency Ultrasonography – this site is a great go-to for providing the foundation for a basic understanding of Emergency Ultrasound through lectures, modules, testing
EMSono – a great site which is a comprehensive emergency ultrasound education website that also provides you with free teaching modules through the SonoBridge. It also provides the ACEP test for bedside US.
SonoGuide – An excellent free online site to learn all that there is to know with regard to bedside US
SoundBytes – a great CME download and set of lectures !
Ultrasound Podcast – a very fun and cool way to learn bedside US through two very funny guys! They also bring you the iPhone app: 1-Minute Ultrasound
Ultrasound SHARE – a great site for a library for all the US videos/images you ever want to see!
US Guided Nerve Blocks – a complete source for all you want to knwo in regard to US guided Nerve blocks.
ViewSono – great video tutorials are short format case based reviews of core ultrasound procedures in emergency medicine, critical care and regional anesthesia
Vimeo US images and videos – an awesome site to see every US related video you’ll ever want to see!
There are quite a few smart phone apps and iTunes videos that can help while you are on the run, train, plane, or riding in the back of a harley:
Dr. Chris Fox’s Emergency US lectures
SonoCase: Motorcycle victim: needs OR! But wait…
So, this case that I just had the other day is an example of an “oldy but goody” reason why bedside ultrasound rocks, especially in the blunt trauma victim with multiple injuries. 40 year-old motorcycle helmeted driver going moderate speed was T-boned by a car and fell onto his left side. He c/o severe left leg pain and mild left lower back pain, with STABLE (and yes, I mean, stable/normal/not worrisome vitals – HR 72, RR 16, BP 148/90, O2 sat 97%RA) with a clear primary trauma survey, and a secondary that revealed a small abrasion on his cheek, no left sided chest wall tenderness, nontender abdomen, no pelvis instability, an obvious deformed open fracture of his left tibia/fibula, and left lower posterior rib cage tenderness without crepitance or bruising. An E-FAST was done… Continue reading
SonoCase: Pediatric lower abdominal bulge? What the…?
You know, working in the pediatric ER is always a joy since most children are going to do well (and most parents are worry warts – but who am I kidding, I would be too!). But sometimes I get a case that surprises me – and this is one of them. Of course, in hindsight, it makes sense, but still interesting given the way the kid presented: 4 year old boy, with a history of “retractable bulges a few years ago” comes to the ER after his mom noticed that he woke up that morning (4 hours prior to arrival) walking funny. She took down his very cute Star Wars pajama pants and saw this: