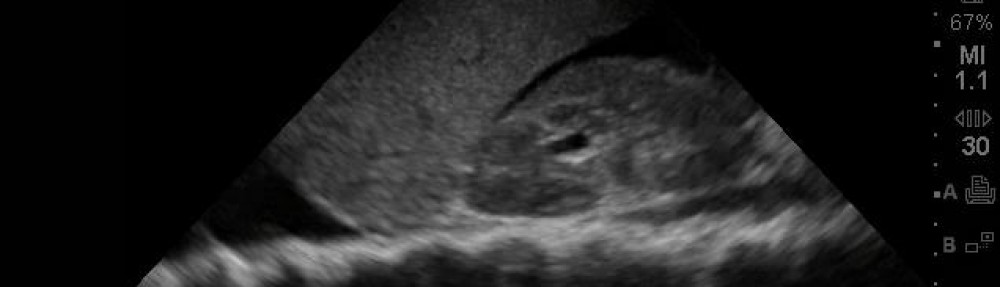
Since it’s RUSH week and we have presented a case yesterday of how the RUSH exam helped show the etiology of unexplained shock in critical situations, I thought Id look through the research before during and after the RUSH exam was described to see where its base was, how it was proven, and what the future of RUSH may hold… Continue reading
Author Archives: SonoSpot
SonoCase: 78 yr old, hypotensive, altered…Welcome to “RUSH” week!
Yup, that’s right, we are going to go through the RUSH exam this week. Its “RUSH” WEEK!!!! To all those in SonoSororities and SonoFraternities out there, this week is going to be dedicated to “rush”ing to evaluate the patients in shock, and trying to figure out the cause of it by your handy-dandy bedside US machine – especially when the case is not obvious, but you know you need to “rush” to their bedside….ok, Ill stop “rush”ing 🙂
RUSH stands for Rapid US in SHock and written by great friends of mine, namely Phil Perera, Tom Mailhot, D Riley, and Diku Mandavia who coined the terms Pump-Tank-Pipies – with inspiration from an original RUSH protocol by another great friend of mine, Scott Weingart (aka emcrit) who coined the acronym HIMAP (heart, IVC, Morison’s (and other FAST views), Aorta, Pneumothroax (see a great podcast by him here). Both start with the heart, and for good reason – you may find the cause immediately, and you’ll be able to identify if the patient can tolerate fluids. Both also arose from varying research studies by Rose et al. (the UHP protocol) and by Bahner et al (Trinity protocol) and Lichtenstein’s FALLS protocol (see thebluntdiessection’s article). Here, we will discuss the 3 sections to evaluate:
SonoFiler: Profiling Dr. Arun Nagdev
The next edition of the Sonofiler – profiling a leader in bedside US – is about a person who is a great friend (and neighbor), an avid researcher in IVC and nerve block US (among other apps), who travels the world teaching US to the masses, and, most importantly, who is just as much of a foodie as I am : Dr. Arun Nagdev. He has plenty of nicknames, none of which I can say publicly (you’re welcome, Arun), but he likes to call himself the “ultrasound dork.” Continue reading
SonoApp: IVC ultrasound – aka “the gift that keeps on giving.”
The IVC is a beautiful thing; it returns blood to the heart from all over the body, and without that, we would die – truly is the gift that keeps on giving. It gives so much information about a patient as it gets affected by so many disease processes:
IVC dilation (hypervolemic)- tamponade, PE, CHF exacerbation, severe mitral regurgitation or aortic stenosis, significant renal failure, severe COPD/Cor Pulmonale
IVC collapsed (hypovolemic) – septic shock, hypovolemic shock, dehydration
Now lets talk technique: Continue reading
SonoStudy (and Case): 53% of septic patients’ treatment plans changed after seeing the IVC and cardiac contractility
The study coming out in Annals of Emergency Medicine in June done by Haydar et al “found point-of-care ultrasonographic data about cardiac contractility, inferior vena cava diameter, and inferior vena cava collapsibility to be clinically useful in treating adult patients with sepsis” – for those of us who use US regularly to evaluate patients in shock, whether it’s by using the RUSH protocol or evaluating the initial and post-fluid volume status for those we are trying to resuscitate when septic, it’s no big surprise. What is the surprising aspect of this is that 53% of septic patients’ treatment plans had changed due to the findings by ultrasound of cardiac contractility and IVC appearance. Continue reading
SonoCase: 25 yr old positional, pleuritic, chest pain. “It’s just pericarditis” Really?
Had a great case the other week of a patient who was previously healthy (“great” because of what it reminds us all to do with this diagnosis) , and other than a girlfriend who he fought with too frequently causing him to go into panic attacks and hyperventilate, he doesn’t have any other stressors in his life – psychologic or drug-induced (yes, I mean cocaine). He came to the ED c/o positional chest pain, worse when lying flat and breathing in, has been persistent for over a week with a recent viral syndrome but no current fever, cough or respiratory distress. He looked well, but felt tired, had no energy to walk a few blocks and that has been worsening over the week, which is when he got into another fight with his girlfriend about coming into the ED for evaluation. Thankfully, he lost and came in. Continue reading
SonoTip&Trick: There’s a left pneumothorax! Really? check again…
Whenever you are performing an E-FAST exam on your trauma patient or a thoracic US in those with unexplained shock or shortness of breath, your sphincter tightens when you see fluid in the belly or when there is no lung sliding. Ever placed your probe on the left anterior chest wall and have been surprised after noticing there is no lung sliding? Or, that you see this weird movement of “the lung” on the left side, which surely isn’t normal and definitely deeper than the pleural line and you think, “There’s a left pneumothorax!” Well, guess what guys and gals, it just could be the heart. Continue reading
SonoFiler: Profiling Dr. Vicki Noble
The next edition of the Sonofiler – profiling a leader in bedside US – is going to be about a person who I admire immensely, has truly changed the way others perceive bedside US, and who was a great president of the ACEP US section: Dr. Vicki Noble – or as we call her “Queen Vicki” – because she keeps a straight face when she needs to and perfectly describes the best utility for bedside US (especially in response to the haters out there… and we all have heard and read what they say). Her response to any and all criticism is always honest and clear – she is my hero. I sent VIcki a few questions, and the answers are so honest, humble, and selfless (and not surprisingly spunky too). They are a true testament as to why she is one of the leaders in bedside US. So let’s talk about how I know that… Continue reading
SonoNews: ASA Guidelines for central venous access now includes ULTRASOUND!
Now I know that many of you may already be using ultrasound to help guide your needle when obtaining central venous access, but when a governing body announces its importance, it’s a big deal! If any of you are like me, you learned how to place all central lines using the “blind” technique – despite your eyes being wide open – but now that the ultrasound machine is your eyes beneath the skin, there is no longer a reason to be so blind about it! Isn’t it nice to know where “big red” is? Here, I’ll answer for you – Heck YEAH! So why am I excited? Well… Continue reading
SonoCase (and studies): Renal colic, do we really need to get another CT?
38 year old male with a history of kidney stones c/o severe right flank pain, radiating to the groin, “feels just like my kidney stones” with small amount of blood in his urine, begging for pain meds. Ok, I know this is not the most mysterious case, but when I looked over his chart he has a radiology list of 8 CT scans over the last 5 years to evaluate for kidney stones! Why? Do we really work in an era where we MUST know the diagnosis instead of just being able to screen for the emergent conditions, and treat by using our clinical judgement… and bedside ultrasound? I sure hope not, because that’s not how I practice. This is not the first-time flank pain patient, although some would argue that you dont need to get a CT for that either if labs and ultrasound are clear/negative. This is also not the elderly patient that could have belly-badness that will die soon – but not from CT scan-radiation-induced cancer, that’s for sure. Continue reading