Author Archives: SonoSpot
SonoTip and Trick: “See” the eye better…Hey ‘bright’ eyes: no pain, no ‘GAIN’!!
Ok, so the “no pain, no gain” doesn’t really make too much sense as the point of this tip and trick is for better visualization of the eyeball : INCREASE THE GAIN! Puts a whole new meaning to the term “Bright eyes.” When you have a patient with painful or painless vision loss, unilateral visual field deficit, trauma to the eye, or if you have a suspicion of a foreign body in the globe – increase the gain – yup, that’s right. Even though the eye is filled with fluid, and fluid is the lover of ultrasound allowing better visualization of structures deep to it on the screen, it can be difficult to visualize WITHIN that fluid filled structure. Lets see some examples: Continue reading
SonoCase: 72 yr old, woke up with “funny” vision… What’s up with that eye?!
One of my good friends and colleagues, Dr. Graham Walker, emailed me the other day with a “booya, check it out”-type of email that he knows I love and cherish. He made the diagnosis quickly with the help of his bedside US study.
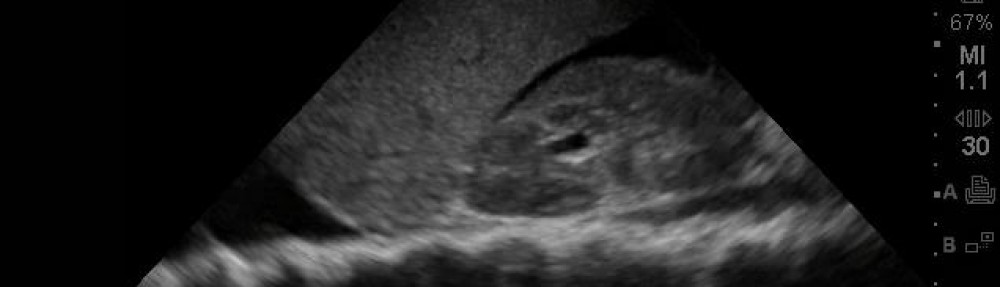
72 year old male with a history of hypertension, high cholesterol and on antibiotics for a foot infection – – stating he woke up and his vision was “funny” – Continue reading
SonoCase: 2 yr old walking into things, now cups his eye to focus…. What’s up with that eye?!
Very cool pick-up we had recently, the early diagnosis allowed better outcome, and I’ve only seen this twice before by bedside US in the ED. It was an unusually calm Monday in the pediatric ER, lots of coughs and colds, and more hand-foot-mouth disease than ever recorded in history, Im sure. Then we saw this very cute 2 year old boy walk into the ER wearing a “Poop happens” T-shirt, with his hand covering his left eye while walking to the room, then hopping on the gurney and immediately taken by the iPAD we have for kids to play games on…. Continue reading
SonoApp: Lung Ultrasound… Be fine with B lines!
So you get a patient with shortness of breath, and you have no idea what the reason is…. but they can’t lie flat and the Xray tech is busy with the trauma. Lung US can help you – but that’s weird, right? Air is supposed to be the enemy of ultrasound with gas scatter artifact making what you want to see very hard. Well, believe it or not, with the lung, ultrasound will turn into your go-to tool for quick evaluation. There has been a study that has described a methodical approach to this, the RADIUS study, and one of the key elements of this is evaluating artifact. Yup, that’s right, ARTIFACT…. Continue reading
SonoNews! – The AMA has passed a resolution in regards to bedside US – thanks to Blaivas et al!
This is HUGE news! Does it change things at all… no. But, does it help our cause? YES! Back in the day, the AMA passed a resolution stating that ultrasound was as tool that can be widely used whose specific use and application should be defined by each specialty with specific hospital privileging. That was a HUGE step for OBGYNs, cardiologists, trauma surgeons, and emergency physicians to take it and run with it, defining ultrasound in a way that was specific to each of those specialties, with more guidelines being thought of for critical care, internists/hospitalists, and ambulatory care doctors. Well, this week, with the help of Dr. Michael Blaivas and others, the AMA passed another resolution, amending the prior stating that ultrasound is a safe, effective and efficient tool, that should be used throughout medical education. This is great for those attempting to incorporate bedside US into their school of medicine. Awesome!!!!
SonoApp: Lung Ultrasound – The down low of pneumo…with the help of Lichtenstein, of course
Lung ultrasound (aka thoracic US) is one of the currently most popular applications of bedside ultrasound. It was found to be more sensitive and specific than chest XRay for pleural effusion, pulmonary edema, and pneumothorax evaluation (see meta-analysis in Chest here)…. how about them apples?! There have been some recent studies suggesting that in the heat of the moment for trauma patients, the sensitivity may be slightly lower than other studies state, but it is still better than chest Xray! Not only does it take a long time to get that chest Xray done in your ED or in through your ambulatory care practice, but its more expensive than bedside limited ultrasound for the patient as well…. lets not even talk about the radiation (yes, I know, Chest Xray radiation is minimal, but it’s still radiation). The evaluation of the lungs takes no more than 3 minutes, and ultrasound machines can be found in your pocket now (should you want that kind of VERY COOL technology). US machines can also be the size of a laptop with better resolution and multiple probe capabilities – so, needless to say, its easy, portable, fast, and more accurate. Now let’s talk… Continue reading
SonoStudy: Lung Ultrasound by Blaivas….. yup, there is a God!
If anyone following SonoSpot does not know who Dr. Michael Blaivas is, you should. As the Greeks have varying Gods for varying reasons, he basically is one of the Gods of point-of-care US. On this current issue of the Journal of US in Medicine by AIUM, he discusses lung ultrasound and its ability to diagnose pneumonia.
SonoCase: 45 yr old female acute respiratory distress…. RUSH, part deux
Here’s another crazy case I had in the middle of the night in the ED, a night that was particularly… let’s say… challenging. Lots of patients (about 43 actually) and 2 thankfully great residents, and one other ED attending. We were busy supervising a chest tube placement, while overseeing the trauma next door and finishing our charts on other patients so they can be dispo’d (yup, multi-tasking at its best – [or worst, ya never know]) and we get a ring down of a 45 year old in acute respiratory distress placed on non-rebreather with subsequent vitals: HR 130s BP 80s/50 RR 38 90%O2 sat. Continue reading
SonoStudy: JAMA – use of CT and MRI increased – everyone saying to watch out!… and be careful…
SonoStudy? well, it’s an indirect sono-related study (and had to interrupt RUSH week) – JAMA article – use of CT and MRI on the rise (CTs have tripled, MRIs have quadrupled!), and thus radiation. The amount of high and very high dose radiation doubled in the last 15 years!! One of the authors stated: “scan rates in the HMOs in the study were a bit lower than in traditional fee-for-service systems, but the growth rates were the same” The reason they suggest: Expanding indications, patient and physician demand, medical uncertainty, and defensive medicine. ok, two words: cancer risk. Plus, in the new era of health care cost control, its time we all start considering the different options: ultrasound (oh yeah!), 1 day rechecks, observation period/stay, or just discharge them with great return precautions if they are low risk/suspicion. This is just insane. view the article: