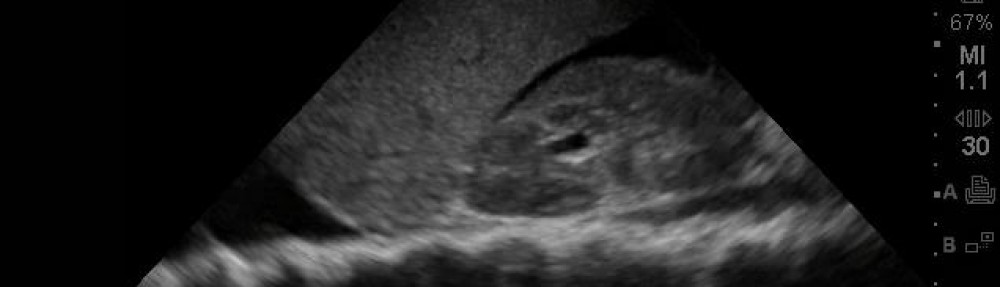
38 year old male with a history of kidney stones c/o severe right flank pain, radiating to the groin, “feels just like my kidney stones” with small amount of blood in his urine, begging for pain meds. Ok, I know this is not the most mysterious case, but when I looked over his chart he has a radiology list of 8 CT scans over the last 5 years to evaluate for kidney stones! Why? Do we really work in an era where we MUST know the diagnosis instead of just being able to screen for the emergent conditions, and treat by using our clinical judgement… and bedside ultrasound? I sure hope not, because that’s not how I practice. This is not the first-time flank pain patient, although some would argue that you dont need to get a CT for that either if labs and ultrasound are clear/negative. This is also not the elderly patient that could have belly-badness that will die soon – but not from CT scan-radiation-induced cancer, that’s for sure. Continue reading
Category Archives: SonoStudies
SonoStudy: US-Guided Nerve Blocks – in disasters, your ED, and your hearts
Given this memorial day weekend, and the sacrifice of our troops, lets discuss something that the military has used for years – and for good reason. US-guided nerve blocks are becoming more and more utilized in our EDs. Especially when we have the elderly patient who is in severe pain from a humeral fracture or a femoral neck fracture, and you’d rather not have to watch (and chase) their blood pressure after giving systemic opiates. It is also a great resource in resource-poor areas, like the aftermath of the disaster of the Haiti earthquake. This is all clearly discussed in the article in Annals of Emergency Medicine this month by Drs. Suzanne Lippert, Arun Nagdev, Mike Stone, Andrew Herring, and Robert Norris. Continue reading
Pre-hospital (paramedic) US: Re-appreciating the Golden Hour…
HAPPY EMS WEEK!!!! We so appreciate all that you do! Along those lines…… and along with many others all over the world in years past, at Stanford there has been a 2-part study being done supervised by Drs. Sarah Williams and Jessica Pierog (PEEPS study) and at UCI supervised by Dr. Chris Fox and others (PAUSE protocol) on the prehospital use/acquisition/ interpretation of emergencies visible by bedside US. It is evident (an understatement, actually) that US needs to go into our ambulances. Continue reading
SonoStudy: “US equivocal for appy” To scan or not to scan? THAT is the question…
Interesting topic of discussion and I wonder what the usual plan is at your facilities with regard to US “equivocal and cannot see the appendix”. Apparently, we order too many CTs after that result, and might want to think about an alternative to radiation: observation period. According to one of our Radiology colleagues who is a guru with US, Dr Brooke Jeffrey, and studied this extensively with a goal to minimize radiation: 400 pediatric and adult patients had US to evaluate for appendicitis. Continue reading
SonoStudy: Top Research in Bedside US – the short of breath patient
Very cool review article on the evaluation of the short of breath patient by bedside US…. the RADIUS study – strong name, if I do say so myself…
http://www.scribd.com/doc/93314237/The-Rapid-Assessment-of-Dyspnea-With-Ultrasound-RADiUS