Now I know that many of you may already be using ultrasound to help guide your needle when obtaining central venous access, but when a governing body announces its importance, it’s a big deal! If any of you are like me, you learned how to place all central lines using the “blind” technique – despite your eyes being wide open – but now that the ultrasound machine is your eyes beneath the skin, there is no longer a reason to be so blind about it! Isn’t it nice to know where “big red” is? Here, I’ll answer for you – Heck YEAH! So why am I excited? Well… Continue reading
Category Archives: SonoTutorial
SonoCase (and studies): Renal colic, do we really need to get another CT?
38 year old male with a history of kidney stones c/o severe right flank pain, radiating to the groin, “feels just like my kidney stones” with small amount of blood in his urine, begging for pain meds. Ok, I know this is not the most mysterious case, but when I looked over his chart he has a radiology list of 8 CT scans over the last 5 years to evaluate for kidney stones! Why? Do we really work in an era where we MUST know the diagnosis instead of just being able to screen for the emergent conditions, and treat by using our clinical judgement… and bedside ultrasound? I sure hope not, because that’s not how I practice. This is not the first-time flank pain patient, although some would argue that you dont need to get a CT for that either if labs and ultrasound are clear/negative. This is also not the elderly patient that could have belly-badness that will die soon – but not from CT scan-radiation-induced cancer, that’s for sure. Continue reading
SonoStudy: US-Guided Nerve Blocks – in disasters, your ED, and your hearts
Given this memorial day weekend, and the sacrifice of our troops, lets discuss something that the military has used for years – and for good reason. US-guided nerve blocks are becoming more and more utilized in our EDs. Especially when we have the elderly patient who is in severe pain from a humeral fracture or a femoral neck fracture, and you’d rather not have to watch (and chase) their blood pressure after giving systemic opiates. It is also a great resource in resource-poor areas, like the aftermath of the disaster of the Haiti earthquake. This is all clearly discussed in the article in Annals of Emergency Medicine this month by Drs. Suzanne Lippert, Arun Nagdev, Mike Stone, Andrew Herring, and Robert Norris. Continue reading
SonoCase: Motorcycle victim: needs OR! But wait…
So, this case that I just had the other day is an example of an “oldy but goody” reason why bedside ultrasound rocks, especially in the blunt trauma victim with multiple injuries. 40 year-old motorcycle helmeted driver going moderate speed was T-boned by a car and fell onto his left side. He c/o severe left leg pain and mild left lower back pain, with STABLE (and yes, I mean, stable/normal/not worrisome vitals – HR 72, RR 16, BP 148/90, O2 sat 97%RA) with a clear primary trauma survey, and a secondary that revealed a small abrasion on his cheek, no left sided chest wall tenderness, nontender abdomen, no pelvis instability, an obvious deformed open fracture of his left tibia/fibula, and left lower posterior rib cage tenderness without crepitance or bruising. An E-FAST was done… Continue reading
SonoCase: Pediatric lower abdominal bulge? What the…?
You know, working in the pediatric ER is always a joy since most children are going to do well (and most parents are worry warts – but who am I kidding, I would be too!). But sometimes I get a case that surprises me – and this is one of them. Of course, in hindsight, it makes sense, but still interesting given the way the kid presented: 4 year old boy, with a history of “retractable bulges a few years ago” comes to the ER after his mom noticed that he woke up that morning (4 hours prior to arrival) walking funny. She took down his very cute Star Wars pajama pants and saw this:
SonoCase: TA Pelvic US: What’s up with that Uterus?!
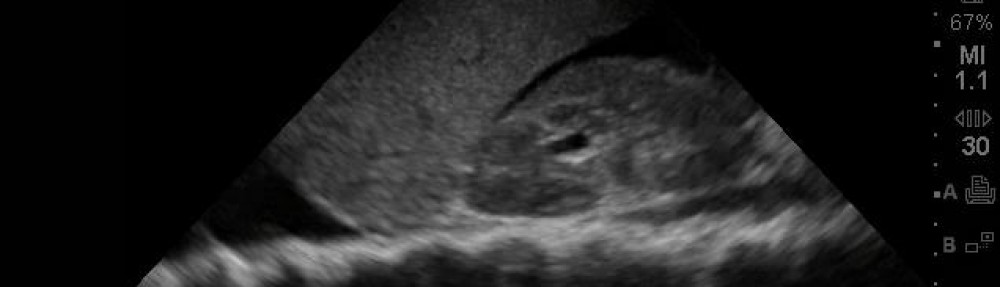
Crazy case I saw recently… 38 yo female who came to the ED for vaginal bleeding that was unrelenting for 6 months, not changed with repeated PO hormonal treatment by PCP, and “I just want an answer.” Stable vitals, no sx of anemia, she was not tender on exam and pelvic was unremarkable except for some blood. In my efforts to simply appease her as I wasnt going to do much more, I did a Transabdominal Pelvic US (sagittal view shown below). Once I saw this, I started to pay more attention (of course, it should have been the other way around, but thats just my skeptical self). I asked her about weight loss (she had 15 pounds loss in 6 months (already a pretty petite girl) and no significant family history, but I realized when speaking to her for more time that she kept having an intermittent dry cough every now and again. I asked her about it, and she thought it was allergies “and I just dont think i got over that cold from a month ago.” Pretty sad case -CXR showed mets…..”platinum” scan done, admitted to Medicine, biopsy/onc/chemo underway… shows the importance of TA Pelvis for not just the 1st trimester pregnancy VB/abd pain evaluations. Continue reading
US for epidurals!
Very Cool illustration page of US for epidurals for my anesthesiology friends by Dr. Chris Mitchell as described by the Broome Docs blog!
Happy Mother’s Day: a dancing baby for all US lovers!
For all the moms out there on Mother’s day! And for all who know me well, you know the baby will be dancin’ to Party Rock! If an expectant mom comes in with pelvic pain or vaginal bleeding, check for fetal dancing: Continue reading
ETT Confirmation by bedside US! Oh yeah….
If the XR tech is busy with the traumas, its the overnight shift where resources are limited, and you just intubated someone who didnt have great breath sounds or O2 sat to begin with – and want to assess if the ETT is in the trachea – cool way to do it. Linear probe. transverse over the trachea at the jugular notch. You will see the the trachea as an arched hyperechoic (bright linear) structure with tracheal rings coming down from it. With the ETT in the trachea, a shadow of the tube over the trachea will be seen, but that may be tough to see at times, so you can put the color doppler box over it and do a little – wiggle wiggle wiggle wiggle wiggle, yeah – of the ETT – a color ray will spike down from the trachea.
SonoCase: “Sent for arthrocentesis” – MSK Ultrasound: How about that tendon?
MSK ultrasound – truly the wave of the future, and current extensive use amongst sports medicine docs who have no XRay machines on the field, and also for disaster and international uses. Someone once said “Problems are to the mind what exercise is the the muscle.” I knew thats why my head hurt during the most recent 49ers playoff game, but I bet their joints were much more sore. Ever wonder what tendonitis looks like on US? Easy and quick diagnosis. Continue reading