Teresa Wu, Associate Residency Director, and Director of Ultrasound and Simulation Programs and Fellowships, for the Maricopa Emergency Medicine Program (otherwise known as “T Wu” – as shouting that loud over and over again gets even the innocent bystanders at the bar chiming in )- has joined her colleague, Brady Pregerson (who manages a free on-line EM Ultrasound Image Library and is the editor of the Emergency Medicine Pocketbook series) once again for a fantastic case highlighted in the recent issue of EP Monthly. Its about a 28 year old female walking in to the waiting room and telling the nurse she has abdominal pain Continue reading
Category Archives: SonoChiefComplaint
SonoCase: 57 yr old with acute chest pain, light-headed….
This case is one of the most interesting cases I have heard about. A true testament to the concept that with bedside US, know what normal looks like well – because if you see something that doesn’t look normal, you may not know what it is sometimes, but it’s not normal and it’s time to explore further. One of our stellar EM residents, Dr. Natatcha Chough, went to the bedside of this patient who was brought by ambulance with appreciable diaphoresis. He was 57 yrs old, c/o gradual onset of chest pressure radiating to his back for 40 minutes (which had resolved after paramedics gave nitroglycerin), feeling light head, with associated shortness of breath, wheezing. He had a history of hypertension and aortic coarctation repaired as a child and at age 20, no history of asthma/COPD, and takes Metoprolol daily.
His vitals: T 36.3 RR 24 HR 83 BP 87/55 O2 sat 93% RA Continue reading
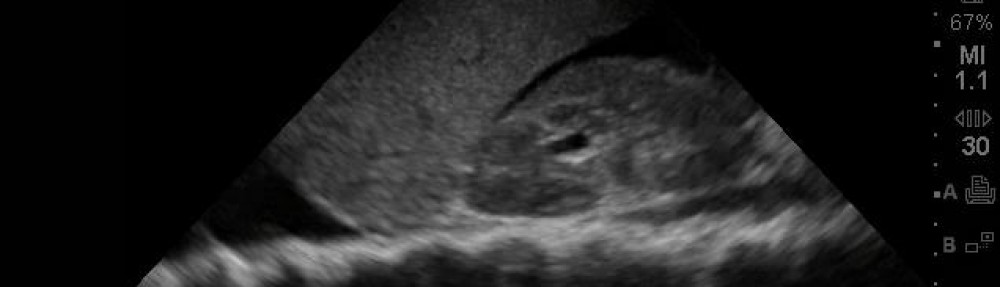
SonoCase: 62 year old male c/o general weakness… you “RUSH” to his bedside…
This case was diagnosed in 10 minutes of patient evaluation according to the resident on our ultrasound elective who performed the scan and the team caring for him in the emergency department. The team knew the diagnosis and, therefore, knew what to order quickly. The patient came with his wife by private vehicle into the triage area of the waiting room where he complained of feeling very weak, more and more over the last 2 days, gradual onset, and said he couldn’t catch his breath with just a few steps. His appetite was poor and wasn’t eating or drinking much, denies chest pain/fever/vomiting/diarrhea or bloody/dark stools. He has a history of metastatic lung cancer (on chemo), diabetes (on insulin), hypertension (on beta blocker), CHF (on lasix), and DVT (on Coumadin) – yeah, I know, survival of the fittest! From what I heard, he did have a smile on his face, so at least he had that going for him, which is so amazing to me – if only we could all be like that!
His vitals: T 36.7 RR 18 HR 90 BP 88/60 O2 sat 93% RA; code status: Continue reading
SonoCase: 75 year old coming in unresponsive…
This case highlights an example of how bedside ultrasound can save a life. Period.
It was 330pm. The ring down from EMS was helpful; we knew the equipment we needed to get ready prior to arrival. “75 year old female, last seen normal at 2pm by family found unresponsive on the carpeted ground of her bedroom, O2 sat 94% and placed on 100% non-rebreather (NRB), shallow breaths at 12/min, weak carotid pulses with one IV access and fluids running, HR 120, blood pressure 60/p, ETA 5 minutes.” Intubation equipment, central access kit, arterial line set-up, and ultrasound machine – ready. Upon arrival, EMS states they have no advanced directive (aka full code until proven otherwise – to social worker: “please let us know when family arrives.”
In the ED… Continue reading
SonoCase: “My back hurts, I just need a med refill.” Yeah, except….
This case scares me. Truly. We have all had patients with this chief complaint, maybe on a weekly, if not daily, basis. You know the one – guy comes in, says he has been diagnosed with …. lets see, its usually “herniated disk”, “muscle strain”, “sciatica”, or he may throw out a term that gets more of your attention like “stenosis”, but usually it’s just “I have a bad back” and now on narcotics (because there’s just no other way – ugh!) and just needs a refill. He may even have an empty bottle in hand. He just might ask for the medicine by name : “Norco 10s work really well, but my doctor put me on Oxycontin now. Can you give me enough for a month?” Response: “uh… No.” But I digress…..lets go to our crazy-scary case…
SonoCase: 72 yr old, woke up with “funny” vision… What’s up with that eye?!
One of my good friends and colleagues, Dr. Graham Walker, emailed me the other day with a “booya, check it out”-type of email that he knows I love and cherish. He made the diagnosis quickly with the help of his bedside US study.
72 year old male with a history of hypertension, high cholesterol and on antibiotics for a foot infection – – stating he woke up and his vision was “funny” – Continue reading
SonoCase: 2 yr old walking into things, now cups his eye to focus…. What’s up with that eye?!
Very cool pick-up we had recently, the early diagnosis allowed better outcome, and I’ve only seen this twice before by bedside US in the ED. It was an unusually calm Monday in the pediatric ER, lots of coughs and colds, and more hand-foot-mouth disease than ever recorded in history, Im sure. Then we saw this very cute 2 year old boy walk into the ER wearing a “Poop happens” T-shirt, with his hand covering his left eye while walking to the room, then hopping on the gurney and immediately taken by the iPAD we have for kids to play games on…. Continue reading
SonoCase: 45 yr old female acute respiratory distress…. RUSH, part deux
Here’s another crazy case I had in the middle of the night in the ED, a night that was particularly… let’s say… challenging. Lots of patients (about 43 actually) and 2 thankfully great residents, and one other ED attending. We were busy supervising a chest tube placement, while overseeing the trauma next door and finishing our charts on other patients so they can be dispo’d (yup, multi-tasking at its best – [or worst, ya never know]) and we get a ring down of a 45 year old in acute respiratory distress placed on non-rebreather with subsequent vitals: HR 130s BP 80s/50 RR 38 90%O2 sat. Continue reading
SonoCase: 78 yr old, hypotensive, altered…Welcome to “RUSH” week!
Yup, that’s right, we are going to go through the RUSH exam this week. Its “RUSH” WEEK!!!! To all those in SonoSororities and SonoFraternities out there, this week is going to be dedicated to “rush”ing to evaluate the patients in shock, and trying to figure out the cause of it by your handy-dandy bedside US machine – especially when the case is not obvious, but you know you need to “rush” to their bedside….ok, Ill stop “rush”ing 🙂
RUSH stands for Rapid US in SHock and written by great friends of mine, namely Phil Perera, Tom Mailhot, D Riley, and Diku Mandavia who coined the terms Pump-Tank-Pipies – with inspiration from an original RUSH protocol by another great friend of mine, Scott Weingart (aka emcrit) who coined the acronym HIMAP (heart, IVC, Morison’s (and other FAST views), Aorta, Pneumothroax (see a great podcast by him here). Both start with the heart, and for good reason – you may find the cause immediately, and you’ll be able to identify if the patient can tolerate fluids. Both also arose from varying research studies by Rose et al. (the UHP protocol) and by Bahner et al (Trinity protocol) and Lichtenstein’s FALLS protocol (see thebluntdiessection’s article). Here, we will discuss the 3 sections to evaluate:
SonoStudy (and Case): 53% of septic patients’ treatment plans changed after seeing the IVC and cardiac contractility
The study coming out in Annals of Emergency Medicine in June done by Haydar et al “found point-of-care ultrasonographic data about cardiac contractility, inferior vena cava diameter, and inferior vena cava collapsibility to be clinically useful in treating adult patients with sepsis” – for those of us who use US regularly to evaluate patients in shock, whether it’s by using the RUSH protocol or evaluating the initial and post-fluid volume status for those we are trying to resuscitate when septic, it’s no big surprise. What is the surprising aspect of this is that 53% of septic patients’ treatment plans had changed due to the findings by ultrasound of cardiac contractility and IVC appearance. Continue reading