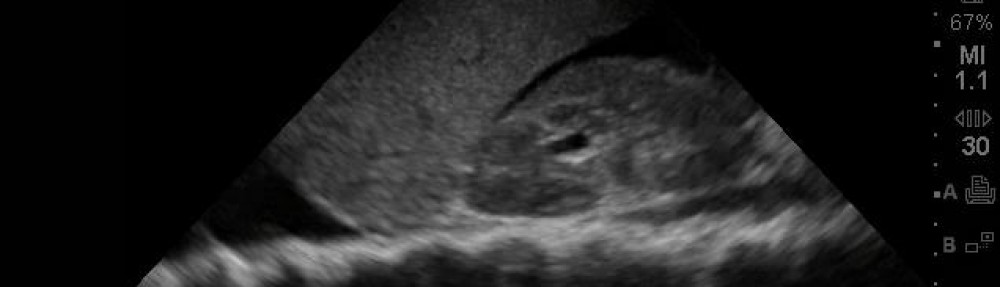
This case was diagnosed in 10 minutes of patient evaluation according to the resident on our ultrasound elective who performed the scan and the team caring for him in the emergency department. The team knew the diagnosis and, therefore, knew what to order quickly. The patient came with his wife by private vehicle into the triage area of the waiting room where he complained of feeling very weak, more and more over the last 2 days, gradual onset, and said he couldn’t catch his breath with just a few steps. His appetite was poor and wasn’t eating or drinking much, denies chest pain/fever/vomiting/diarrhea or bloody/dark stools. He has a history of metastatic lung cancer (on chemo), diabetes (on insulin), hypertension (on beta blocker), CHF (on lasix), and DVT (on Coumadin) – yeah, I know, survival of the fittest! From what I heard, he did have a smile on his face, so at least he had that going for him, which is so amazing to me – if only we could all be like that!
His vitals: T 36.7 RR 18 HR 90 BP 88/60 O2 sat 93% RA; code status: Continue reading →
 -from Medicineo blog
-from Medicineo blog