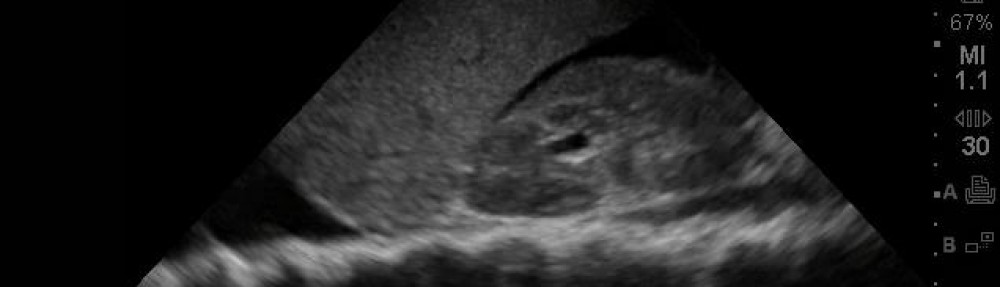
This case was quite interesting and a great pick-up by the EM resident, Dr Cesar Avila. It highlights the use of ocular ultrasound with eye complaints/vision change/trauma, especially when you cannot properly evaluate the eye well due to eyelid swelling.
82 year old male with history of globe rupture and retinal detachment status post repair two months earlier presents to the ED with eyelid swelling of that same eye, gradual onset over one day with now inability to open eyelids well with yellow discharge coming from eye. Continue reading