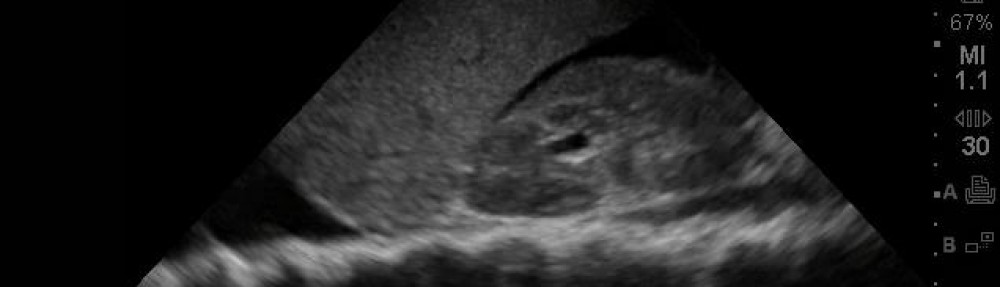
This case is one of those cases that make me so proud of the residents I work with…. Drs. Brianne Steele and Cesar Avila identified the need for a RUSH exam, but didn’t stop there – they noticed something during their RUSH and proceeded with another evaluation – obtaining the surprising diagnosis below, saving him time in the emergency department and canceling his CT scan that didn’t need to be done, which I then conclude controls his healthcare charge. period.
70 year old male with a history of (ready for it…) Continue reading